Free download: Top 10 Natural & Easy Remedies for Joint Pain from Home. Learn these helpful remedies.
Estimated Reading Time: 11 minutes read
Have you heard of the phrase going “weak in the knees?”… Well, you can go weak in the ankles too!
Chronic ankle instability can be a very challenging condition to deal with if you’re not sure what to do.
While the term chronic does mean it’s an ongoing issue, there are still ways to effectively manage chronic ankle instability and help you live a normal life.
Table of Contents
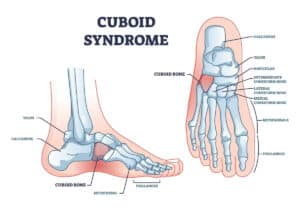
What Is Chronic Ankle Instability?
If an initial ankle sprain doesn’t heal after a certain time frame or a recurrent sprain/sprains occurs within a certain time frame, then you’re at high risk of developing chronic ankle instability.
The exact timeline of officially diagnosing an ankle sprain or ankle instability as chronic may vary. Some sources consider an accurate chronic ankle instability diagnosis if a sprained ankle hasn’t healed or has recurred again within 6 weeks of the initial injury.
Other sources indicate that if a severe ankle sprain has not healed or has recurred within a time frame of 6 months, then it’s considered an unstable ankle.
Keeping in mind that an ankle sprain is ultimately an overstretching of the ligament fibers or, if more severe, can involve an actual torn ligament, repeated ankle sprains or an ankle sprain that never fully healed has the potential to create permanent ligamentous laxity.
As the term implies, ligamentous laxity creates weakness and instability in the ankle. This places you at a higher risk for further injury and can make any weight bearing tasks more challenging.
All in all, over an extended period of time, if you are continuing to experience recurrent ankle sprains or have never fully recovered from a previous ankle sprain, then you are at a higher risk to develop chronic ankle instability.
Causes of Chronic Ankle Instability
Chronic ankle instability most commonly occurs as a result of repeated ankle sprains.
An ankle inversion injury is the most common type of ankle sprain to occur. Inversion of the foot and ankle occurs when the ankle rolls towards the outside edge of the foot. This can lead to persistent ankle instability in the lateral ankle ligaments.
Mechanical Instability
Mechanical instability looks at how deviations or changes in your ankle anatomy can make you more prone for ankle sprains and ankle instability. This may include the anatomy you were born with, or anatomical changes that occur as a result of degenerative changes or injuries.
For example, a hindfoot varus or pes cavus (a.k.a. heel inversion and a high arch in the foot) can increase your chances of foot inversion, and therefore, a sprained ankle via an inversion injury.
While foot inversion is the most common direction to suffer an ankle sprain, an eversion injury is also possible. This is when the foot and ankle roll excessively inward in the direction of the arch and can lead to persistent ankle instability in the medial ankle ligaments.
If one is born with hindfoot valgus or pes planus (a.k.a. heel eversion and a flat foot), this can make you more susceptible to an ankle eversion sprain.
Natural wear and tear in the joint, or ankle arthritis, can also affect ankle stability and lead to chronic ankle pain. As the joint continues to degenerate, it’s more common to develop surrounding muscle imbalances and demonstrate a greater challenge in maintaining ankle stability.
It’s important to note that ligamentous laxity itself is considered a mechanical cause of instability, as the injured ligaments have not been able to heal and return to their original supportive state.
Functional Ankle Instability
Functional ankle instability is typically caused by one or more of the following:
- Weak ankles
- Poor postural control
- Poor balance and unsteadiness
- Lack of proprioception
One or more of the above issues can contribute to a lack of support around the ankle joint and make you more susceptible to experience ankle sprains and ankle instability.
Symptoms of Chronic Ankle Instability
If you have experienced a singular severe ankle sprain or multiple prior ankle sprains, and have then developed chronic ankle instability, you may notice one or more of the following symptoms:
- The ankle rolls or gives way in the direction of instability
- Persistent and chronic pain
- Weak ankles
- Swelling
- Difficulty bearing weight on the affected foot (e.g., walking, squatting, climbing stairs), especially on an uneven surface
- Recurrent sprains
Making a Diagnosis of Chronic Ankle Instability
A physical exam by an orthopaedic specialist, who specializes in ankle injuries, will help to confirm a clinical diagnosis of chronic ankle instability.
It’s not uncommon to see an orthopaedic surgeon, such as a foot and ankle surgeon, for this exam, although it doesn’t necessarily mean you automatically need surgery.
The medical professional will perform a physical exam to assess lower extremity range of motion and strength. They will assess any regions that might be tender to touch, such as over the ankle ligaments previously or more recently sprained.
Special orthopaedic tests will provide stability testing of these ligaments as well.
Additional imaging, such as from magnetic resonance imaging (MRI), can help to check the quality of the ankle ligaments and other surround structures, such as the bones, muscles and tendons.
Treatment for Chronic Ankle Instability

A full exam will help determine the course of treatment for your chronic ankle instability. This will involve surgical repair or nonsurgical treatment.
Surgical Repair
When is surgery needed?
After having tried all nonsurgical efforts, if you continue to experience chronic ankle instability, recurrent ankle sprains, and have ongoing pain and functional restrictions, then surgery may be necessary.
The exact surgical repair performed will depend on your surgeon’s specific recommendations based on your individual ankle instability scenario.
Ankle surgeons may consider anatomic reconstruction. According to the Institute for Quality and Efficiency in Health Care, the damaged ligaments may be shortened or tightened.
There is also the possibility of a tendon allograft and use it to replace the damaged ligament. If torn ligaments are present, the surgeon may attempt surgical repair.
These are just a few examples of possible surgical techniques that may be used for treatment of chronic ankle instability.
After a successful surgery, your surgeon may have you on weight bearing restrictions. You may need to use crutches or some other type of assistive device temporarily. An ankle brace may be necessary for a certain time frame as well.
Once cleared, your surgeon will likely refer you to physical therapy to begin your rehab journey. Full recovery can take anywhere from several weeks to several months, depending on your exact surgical procedure.
Nonsurgical treatment
It may be recommended for you to wear an ankle brace when out and about, especially when on uneven surfaces. This can help to support the ankle in order to avoid experiencing further ankle sprains.
Physical therapy is a common nonsurgical treatment approach to help manage an unstable ankle. A physical therapist may perform ankle taping to help support the ankle while you’re re-learning and re-training the ankle to try and support itself.
The following video is a demonstration of a simple self-taping technique you can use as needed to help control your chronic instability.
Physical therapy will also include ankle stabilization exercises, which are key to helping regain control over the unstable ankle.
Let’s take a look at a few exercises that focus on ankle strengthening, neuromuscular re-education, and proprioception training.
Resisted Ankle Eversion


As inversion injury is the most common ankle sprain to experience, this exercise focuses on the lateral ankle ligaments and muscles typically affected, such as the peroneal muscles.
- You can perform this seated in a chair with the affected leg extended in front of you or seated on the floor with your legs stretched in front of you.
- You’ll loop a resistance band (light, medium or heavy resistance) around the ball of foot, holding the ends in your hands.
- Shift and hold the band away from the outside of the foot, while maintaining tension in the band.
- Next, flex the ankle back and wing it out to the side. Hold for 2 seconds, then return to your starting position.
- Repeat 10-15x for 2-3 sets.
Single Leg Balance


- Stand in front of a firm surface (e.g., countertop) in case you need some help to balance.
- Stand on the affected leg and lift the other leg off the floor (make sure to engage your glutes and core to help support you).
- Hold your gaze steady on a set object in front of you to help you balance.
- Practice balancing for up to 30 seconds, rest, then repeat again.
Tip: To make this more challenging, you can advance to practicing on an uneven surface, such as a folded towel. If you have access to gym equipment, you can use a bosu ball, piece of foam or dyna-disc to practice on.
Stationary Forward Lunge


- Stand next to a firm surface in case you need some additional help balancing.
- Take one big step forward, placing the affected leg forward and the other in the back. The front foot should be flat, but the back heel should be lifted off the floor.
- Lower down into a lunge by bending the knees as far as you’re comfortable with. Make sure the front knee remains in line with the ankle.
- Hold for 2 seconds, then return to your starting position.
- Repeat 10x for 2-3 sets.
Tip: If you begin having knee pain with this, make sure to check your positioning and form. You may need to move your feet further apart or together, depending on where you began. You may also want to modify the depth of the lunge.
Standing Tabletop Pose


- Again, stand in front of a sturdy surface in case you need some assistance balancing. Make sure to stand far enough away from the surface so that you have enough room to move into the pose.
- Take a big step forward with the affected leg, reaching for the sturdy surface with your arms.
- As you step forward, lift your back leg and allow the torso to rock forward until your arms, torso and back leg are parallel to the floor.
- Try to hold and balance on your supportive leg for 2 seconds, then return to your starting position.
- Repeat 10x for 2-3 sets.
As this one is a little more challenging, take a look at the following video for a live demonstration showing how to perform it.
Double Leg Calf Raises

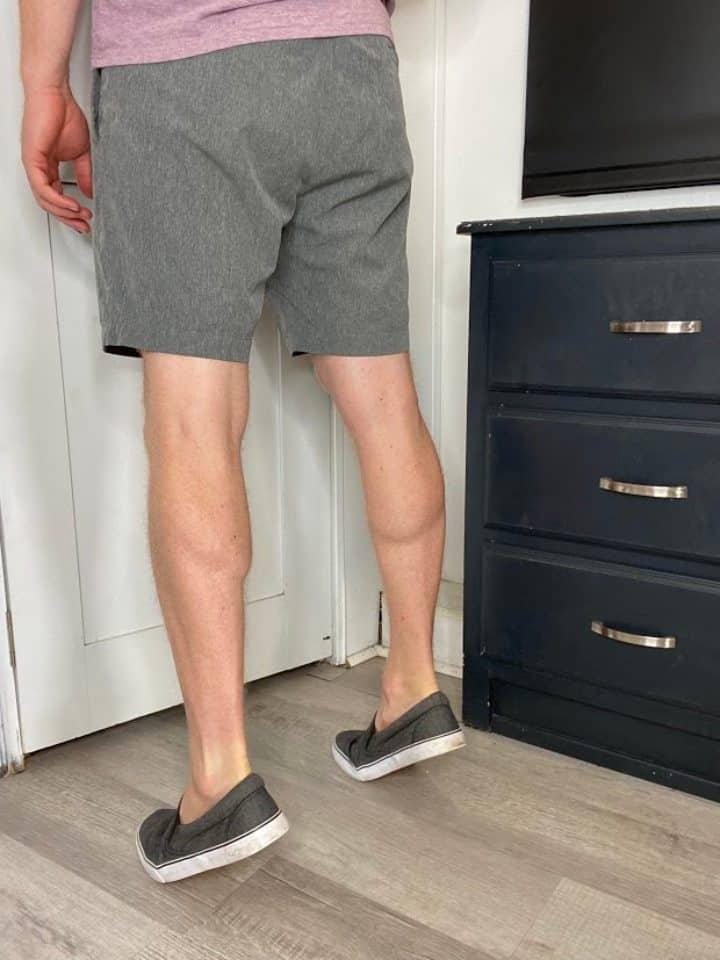
- Standing in front of that sturdy surface again, place your feet side by side a little smaller than hip width apart.
- Slowly lift the heels off the ground, while avoiding rolling of the ankles
- Hold for 2 seconds then return to your starting position.
- Repeat 10-15x for 2-3 sets.
Single Leg Calf Raises


This is a progression from the last exercise.
- Standing in front of a firm surface, stand on the affected leg. Make sure to engage your glutes and core.
- Slowly lift the one heel off the ground, while avoiding rolling the ankle.
- Hold for 2 second.
- Repeat 5-10x for 2-3 sets.
A single leg calf raise can be very beneficial, but quite challenging. It’s important to make sure you don’t force this motion, as you don’t want to cause further pain or a muscle strain.
The following video will demonstrate the right and wrong way to perform a single leg calf raise for clarification.
Long-Term Management of Chronic Ankle Instability
To best manage your ongoing ankle instability, make sure to keep a consistent home and exercise routine.
It’s important to keep the ankle as strong and stable as possible, even with a history of recurrent ankle sprains.
Utilize an ankle brace or ankle taping as needed in order to control pain and promote functional mobility.
Never hesitate to reach out to a healthcare provider if you feel you may need more help than just your home routine to further manage your ankle instability.
FAQ:
Should I use ice or heat with chronic ankle instability?
Seeing as chronic ankle instability is commonly accompanied by swelling, ice would be the best choice to use.
Can I run with chronic ankle instability?
High impact activities, such as running, aren’t the best with chronic ankle instability due to your higher chances of spraining the ankle. If you do choose to run, it would be recommended to wear and ankle brace and avoid uneven surfaces.
Can I get a massage for chronic ankle instability?
Sure! If you have pain and tightness related to your ankle instability, a massage can be very helpful. Always let your massage therapist know about any injuries you have.