Free download: Top 10 Natural & Easy Remedies for Joint Pain from Home. Learn these helpful remedies.
Estimated Reading Time: 11 minutes read
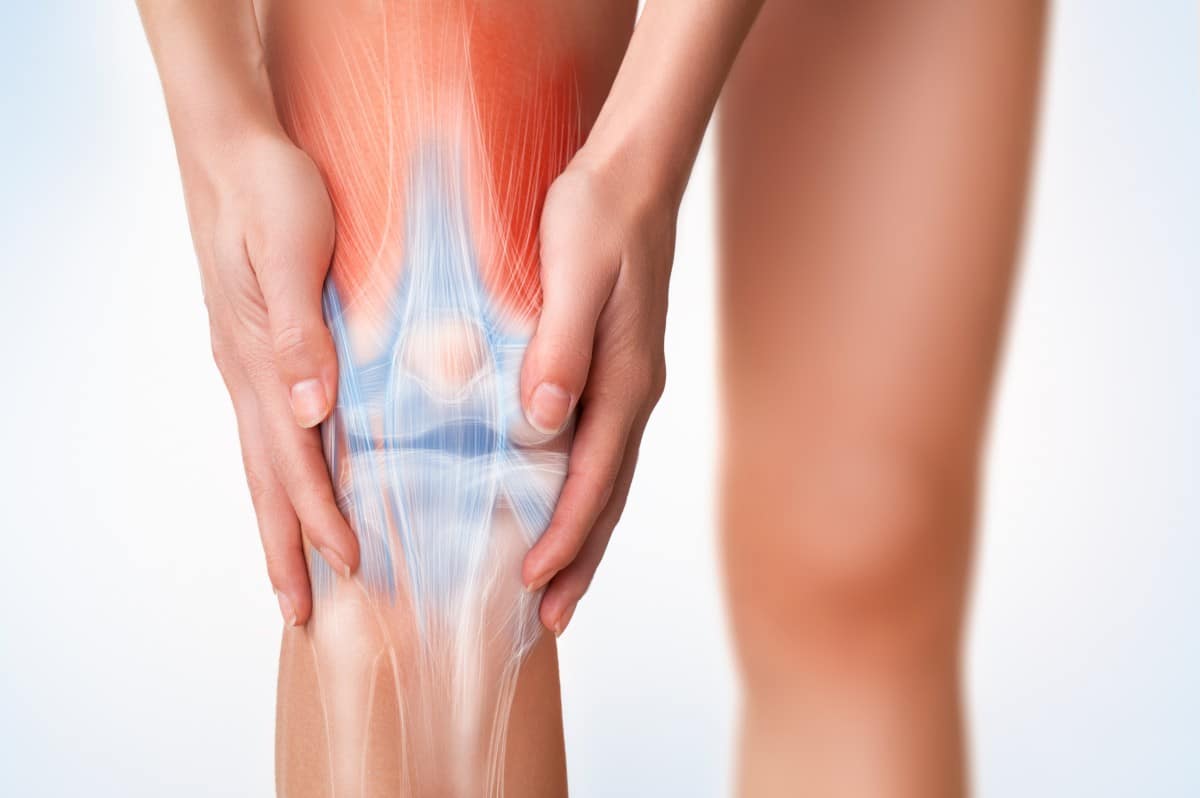
Having a basic understanding of knee anatomy can be extremely beneficial.
The human body is very complex, including the knee which is actually known as a complex joint. When we have pain or injure ourselves, it can be frustrating to not know why this is happening. With basic knowledge of our anatomy, when pain or injuries do occur, we’ll have a better chance of managing the issue or even preventing a problem from occurring in the first place.
This article will focus on anatomy of the knee specifically. Believe it or not, the knee is actually the largest joint in the body!
Table of Contents
The Knee Joint
The knee joint is a hinge joint. It allows for knee flexion and extension, otherwise known as bending and straightening of the knee.
While flexion and extension are the primary motions that occur at the knee, it’s important to note that a few other motions technically occur at the knee as well. There is also a small bit of medial and lateral, or inner and outer, rotation as well as varus and valgus stresses.
Without this hinge joint, we wouldn’t be able to do many of the things we carry out on a daily basis. This includes walking, sitting, standing, squatting, taking stairs, etc.
1. Bony Structures of the Knee
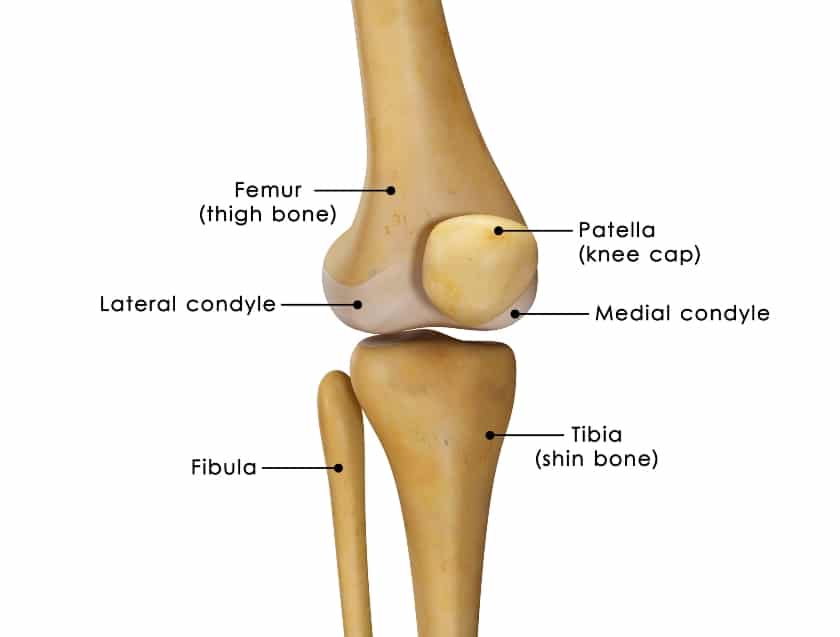
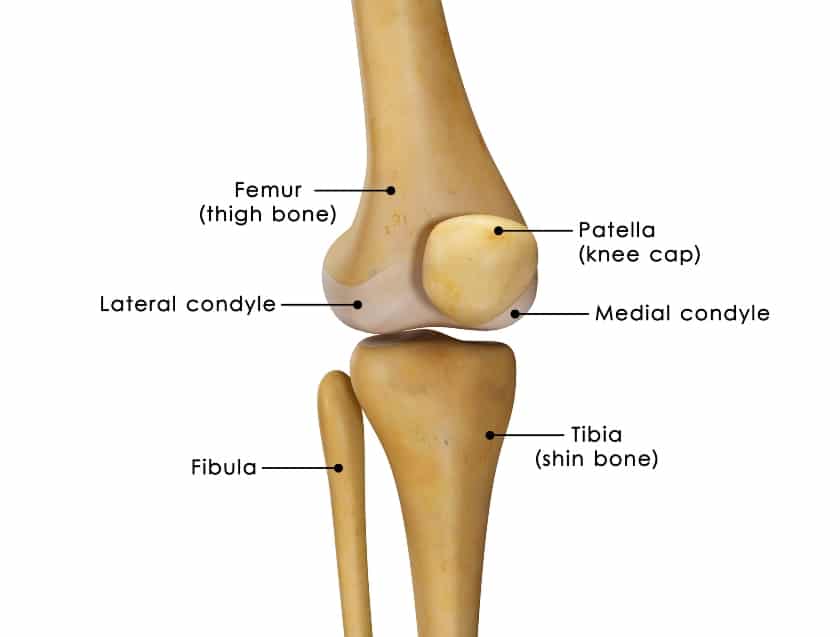
The knee bones consist of the following:
- Femur, or thigh bone
- Tibia, or shin bone
- Patella, or knee cap
These knee bones come together to form two specific articulations:
Patellofemoral joint: Formed via the trochlear groove of the femur (this is where the patella glides) and the posterior or back aspect of the patella.
Tibiofemoral joint: Formed via the joining of the lateral and medial condyle of the femur with the tibial plateau.
It’s helpful to mention the fibula bone. Although this doesn’t directly connect to and form the knee joint, its location on the lateral or outer lower leg next to the tibia is important as multiple muscles and ligaments attach to it. These muscles and ligaments contribute to movement and support at the knee.
2. Knee Cartilage
Cartilage is present on the surfaces of the bony structures that make up the knee joint.
This articular cartilage allows for smooth gliding and cushioning of the bones against each other. This creates a helpful shock absorption at the knee during activities such as walking, running and jumping.
The challenge many will face with knee arthritis is that this essential cartilage begins to wear and break down. Without this important support, pain will typically ensue.
3. Synovial Fluid
Synovial fluid is a lubricating fluid found in many joints. This fluid works with the articular cartilage to provide shock absorption and a smooth gliding motion in the joints.
The synovial fluid also acts as a way for nutrients to move in and out of the joint.
Not only does synovial fluid fill the knee joint space, but it fills in any spaces existing in the cartilage as well.
Movement encourages production of synovial fluid. By staying active and regularly exercising the right way, you’re then providing the knee joint with the synovial fluid it needs to stay lubricated, supported, and have all the right nutrients needed to stay healthy.
4. Knee Bursae
Bursae are fluid-filled sacs commonly found around the joints, including the knee. Bursae are another group of structures that help to reduce friction in the joint, as well as provide extra cushioning and support during movement.
Multiple bursa sacs exist around the knee. Some are directly located around the patella, while others are further away from the patella, but still surround the knee joint itself.
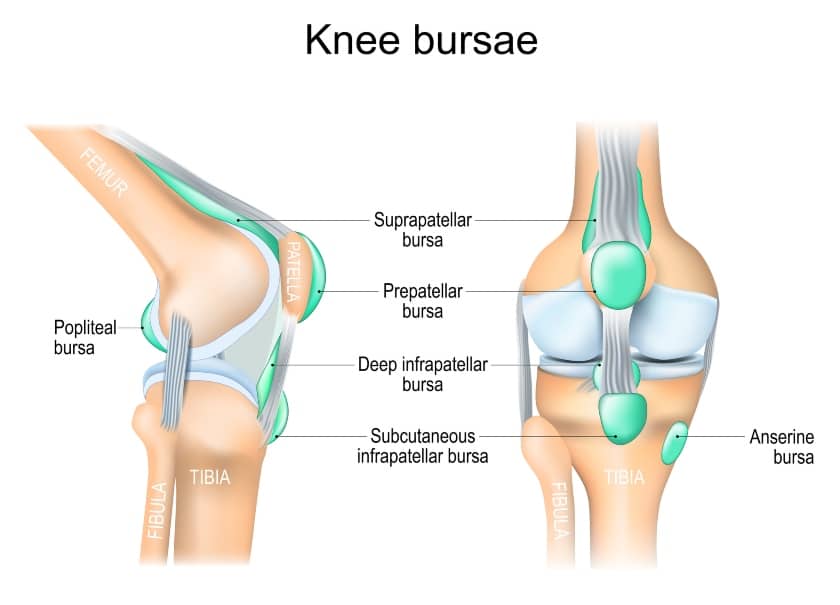
The following are categorized as patellar bursae:
- Prepatellar bursa
- Infrapatellar bursa (superficial and deep)
- Suprapatellar bursa
The following bursae are not specifically located at the patella, but nearby areas around the knee:
- Pes anserine bursa
- Iliotibial bursa
- Gastrocnemius-semimembranosus bursa
- Medial collateral ligament bursa
- Lateral collateral ligament bursa
When the bursae become inflamed or irritated, this commonly leads to painful knee bursitis.
5. Knee Ligaments
Ligaments connect bone to bone. They are vital in providing support and stability to any joint. Injury to any of these ligaments leads to a significant lack of support, instability and pain in the knee.
The following are the most well-known ligaments that support the knee joint:
- Anterior cruciate ligament (ACL)
- Posterior cruciate ligament (PCL)
- Medial collateral ligament (MCL)
- Lateral collateral ligament (LCL)
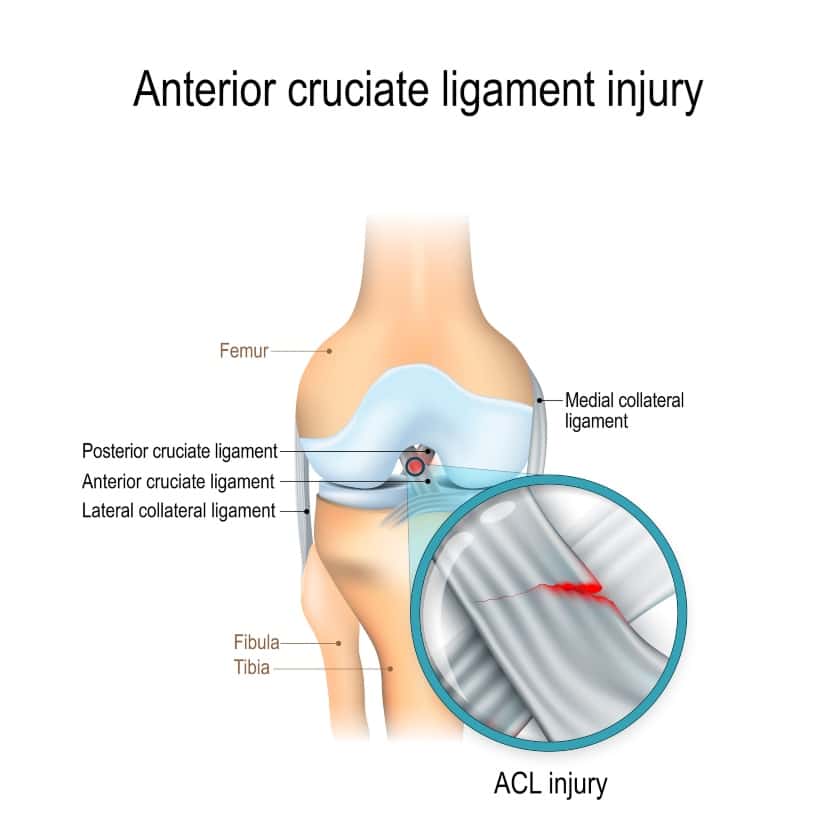
A. Anterior Cruciate Ligament
The ACL is one of two cruciate ligaments located in the front of the knee. It connects from the lateral femoral condyle to the intercondylar region of the tibia.
The ACL connects the femur or thigh bone to the tibia and prevents excessive anterior or forward translation of the tibia. It also prevents excessive rotational forces.
B. Posterior Cruciate Ligament
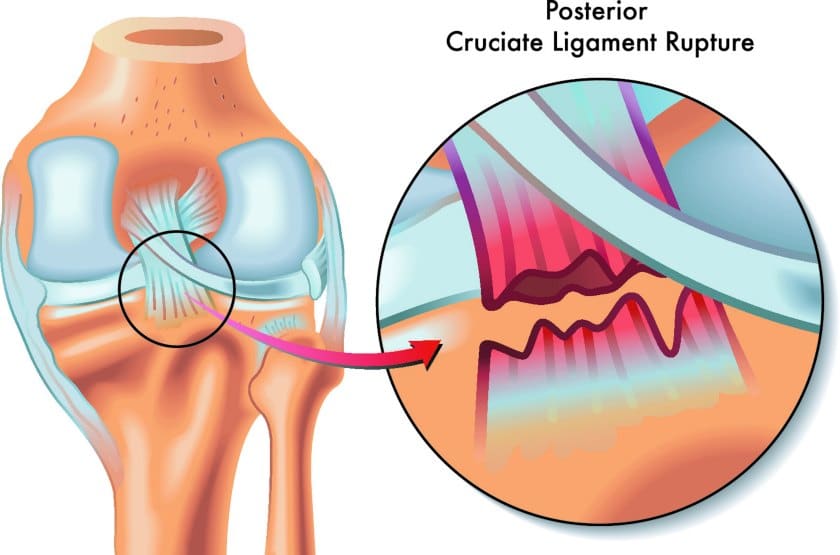
The PCL is the other cruciate ligament located in the back of the knee. It’s actually considered stronger than the ACL, with the ACL more commonly injured.
The PCL runs from the medial femoral condyle to the posterior or back of the tibia.
The PCL connects the femur and tibia as well. Its role is to prevent excessive posterior or backward translation of the tibia. Like the ACL, the PCL also prevents excessive rotational forces from occurring at the knee.
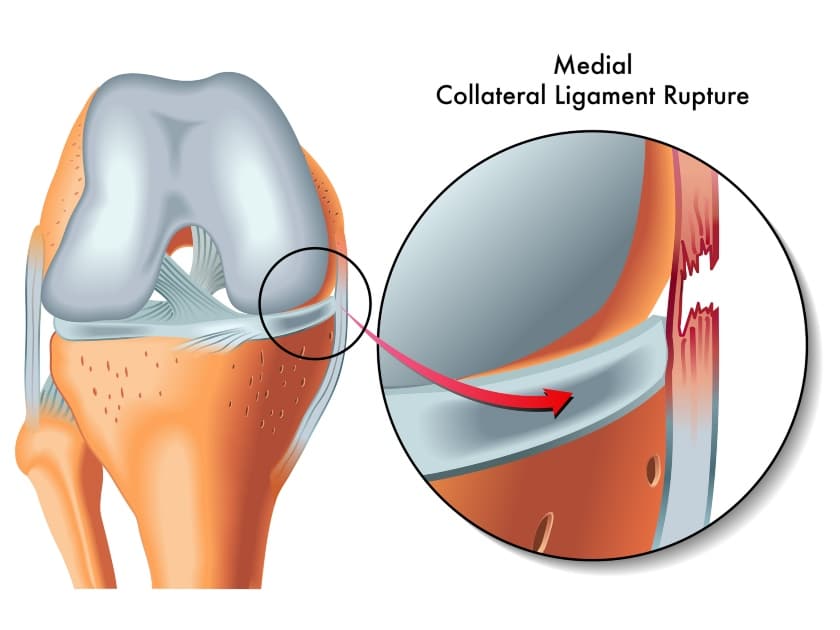
C. Medial Collateral Ligament
The MCL connects the medial epicondyle of the femur to the medial condyle of the tibia. It consists of a superficial and deep layer.
The MCL is one of two collateral ligaments. It supports and stabilizes the medial or inner aspect of the knee.
It helps to prevent excessive valgus or medial forces while bending and straightening the knee, although this prevention of these forces is most successful when the knee is fully extended. The MCL also helps to prevent excessive external rotation at the knee joint.
D. Lateral Collateral Ligament
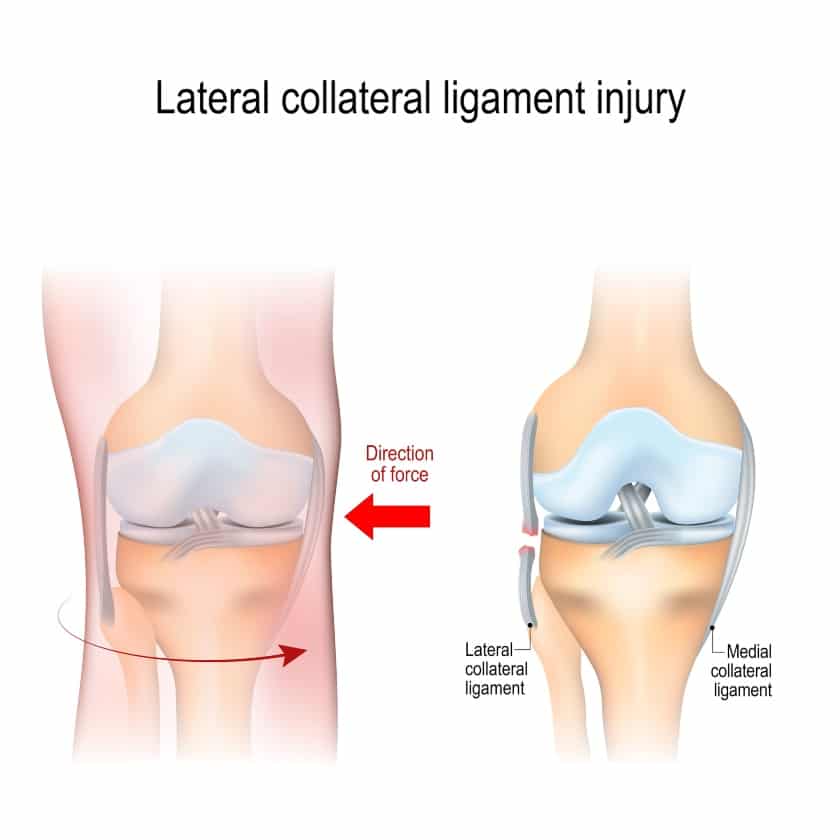
The lateral (fibular) collateral ligament connects from the lateral femoral epicondyle to the head of the fibula.
The LCL is important for stabilizing the lateral or outside aspect of the knee.
It prevents excessive varus or lateral forces at the knee, as well as excessive lateral or external rotation of the tibia shin bone.
E. Other Ligaments to Consider
Other not so well-known ligaments that assist in providing additional support and stability to the knee include the following:
Arcuate Popliteal Ligament: This connects from the lateral fibula to the posterior or back of the knee. This ligament helps to avoid and prevent knee hyperextension.
Oblique Popliteal Ligament: This connects extends from one of the hamstring tendons, semimembranosus. This tendon connects from the medial tibial condyle to the lateral femoral condyle. It helps to provide additional posterior support of the knee.
Fabellofibular Ligament: While the name sounds made up, this is an actual ligament in the knee. This ligament runs next to the LCL and helps to prevent excessive varus, lateral rotation, and posterior motions at the knee.
Popliteofibular Ligament: This ligament connects from the popliteus muscle to the to the fibula. It helps to prevent excessive posterior and lateral rotation forces.
While these ligaments don’t usually get as much attention as the cruciate and collateral ligaments, they are still important structures that help in stabilizing the knee, and therefore, deserve recognition.
6. Knee Menisci
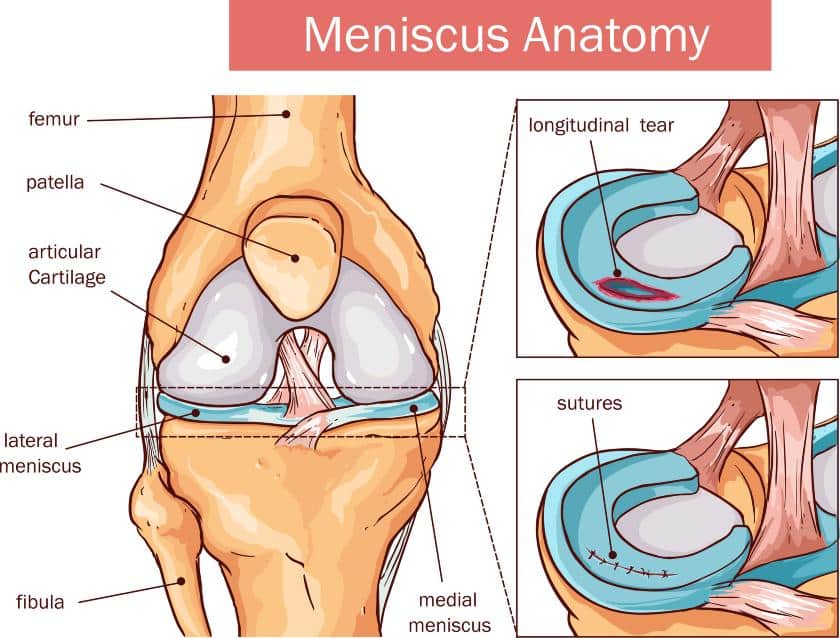
Two menisci are situated in the knee joint:
- Medial meniscus
- Lateral meniscus
The medial meniscus, as its name implies, is located on the medial or inner knee. The lateral meniscus is located on the lateral or outer side of the knee.
The menisci act as shock absorbers and reduce impact during movement. They additionally stabilize and support the knee joint like many of the other soft tissue structures around and in the knee.
Wear and tear in the menisci and cartilage will typically have an effect on each other and can lead to painful friction forces in the knee.
7. Knee Plica
Not many are aware of the anatomical structure known as plica. A plica is a fold in the synovial membrane.
There are four plicae in the knee joint:
- Suprapatellar
- Infrapatellar
- Medial
- Lateral
The purpose of plicae is for extra support and protection of the knee. When these get irritated, plica syndrome will develop. This can cause pain and inflammation in the knee, limiting range of motion and functional movement.
8. Knee Fat Pads
Fat pads are located in the front, or anterior, aspect of the knee cap. They are also known as Hoffa’s fat pads.
The fat pads are also shock absorbers for the knee during regular movement and help to cushion the knee cap. There are many nerves in the fat pads, so any injury or damage to them can be very painful.
9. Muscles and Tendons of the Knee
There are a TON of muscle and tendon attachments to the knee. Contractile forces from muscles transmit through their attaching tendons, which connect muscle to bone, and this allows joint movement.
Let’s take a look at the primary muscle-tendon units that connect to the knee joint.
A. Quadriceps
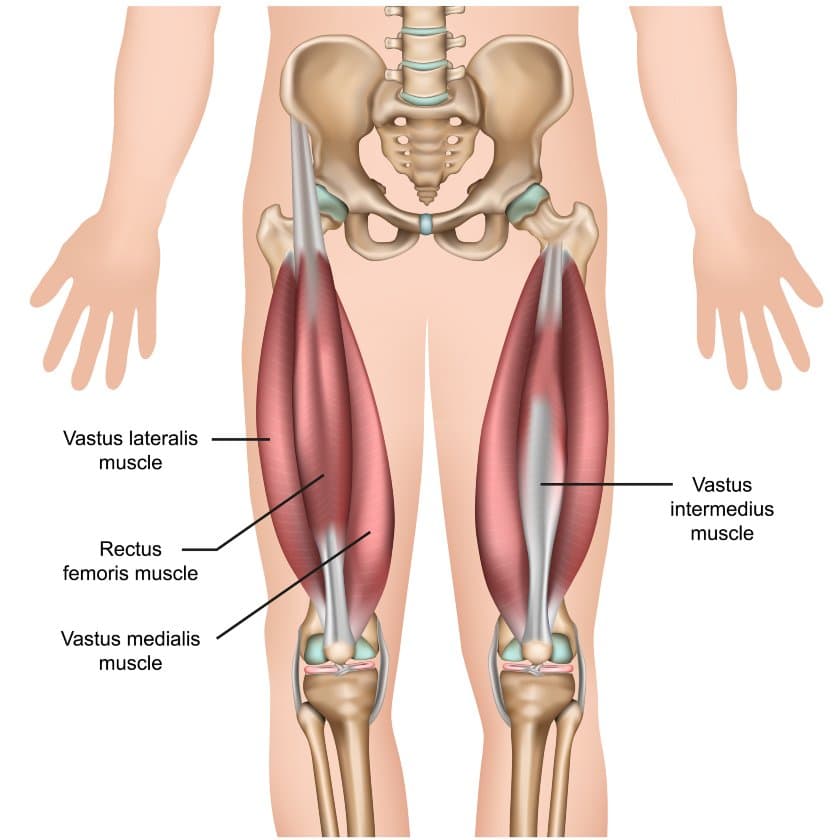
The quadriceps, or quads, are made of 4 muscles located in the front of the thigh. These muscles merge together to form the quadriceps tendon:
- Rectus femoris
- Vastus lateralis
- Vastus medialis
- Vastus intermedius
The quads’ action at the knee involves extending or straightening the knee.
The quadriceps tendon attaches to the top of the patella. When the knee straightens, it glides the patella in an upward or superior direction.
B. Hamstrings
The hamstrings consist of three muscles located in the back of the thigh. Each of these muscles has their own tendon attachment to the back of the knee:
- Biceps femoris
- Semitendinosus
- Semimembranosus
These muscles are primarily responsible for flexion or bending of the knee.
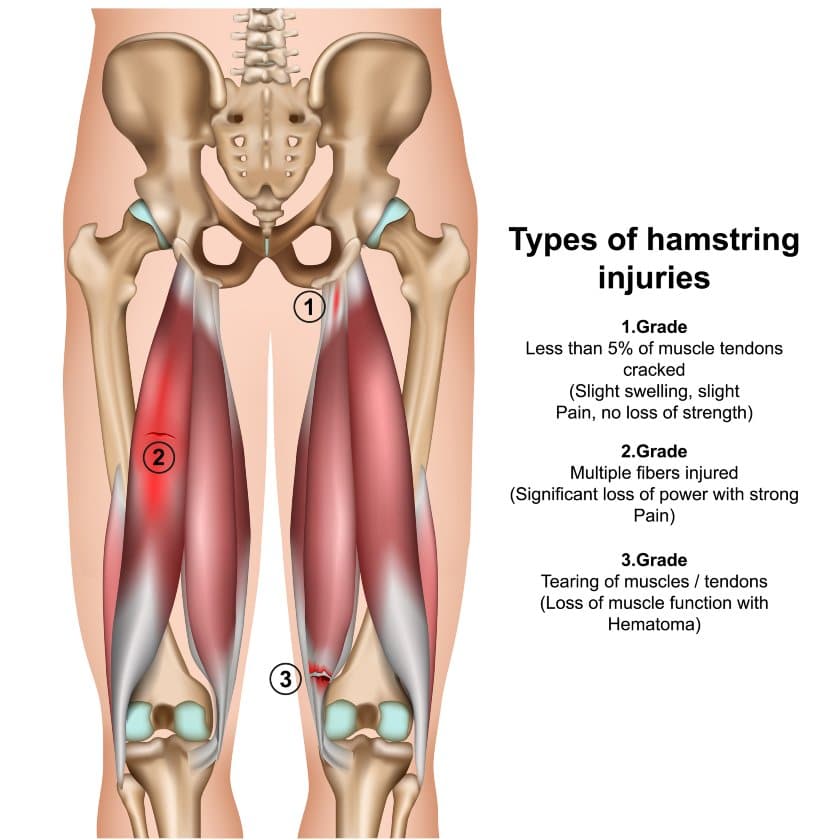
The biceps femoris is the outermost or lateral hamstring muscle, connecting to the fibular head.
Semitendinosus and semimembranosus are located more medially compared to the biceps femoris. Semitendinosus inserts at the pes anserine on the tibia, whereas semimembranosus connects to the medial condyle of the tibia.
C. Gastrocnemius
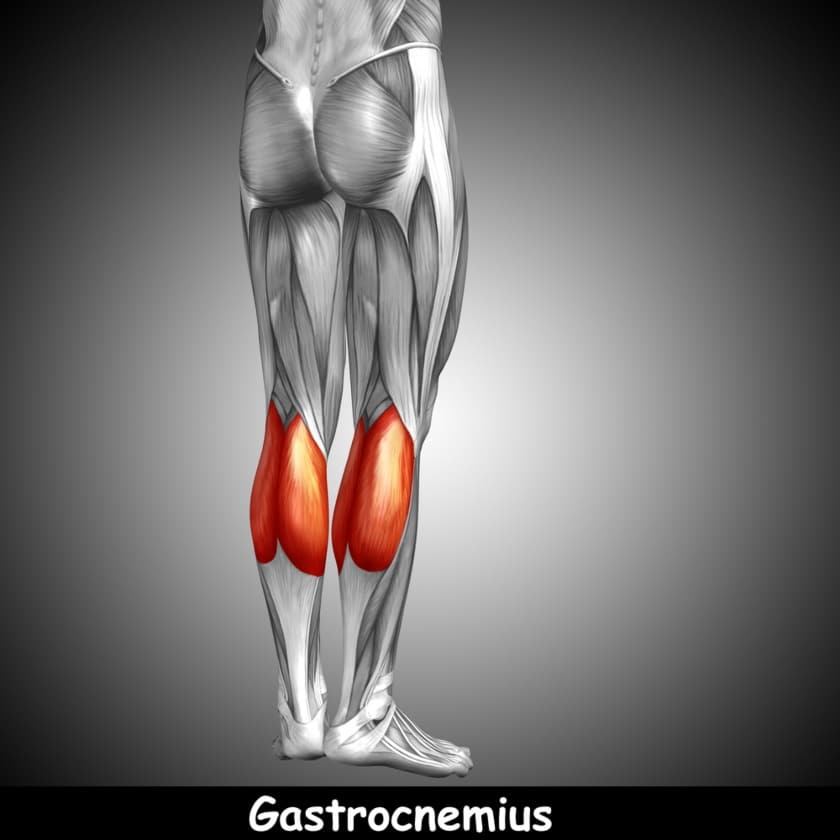
Gastrocnemius is the primary muscle that makes up what we know as the calf.
It has two heads: medial and lateral. The medial head attaches to the medial femoral condyle, while the lateral head attaches to the lateral femoral condyle.
At the knee, the gastrocnemius is responsible for assisting in knee flexion or bending.
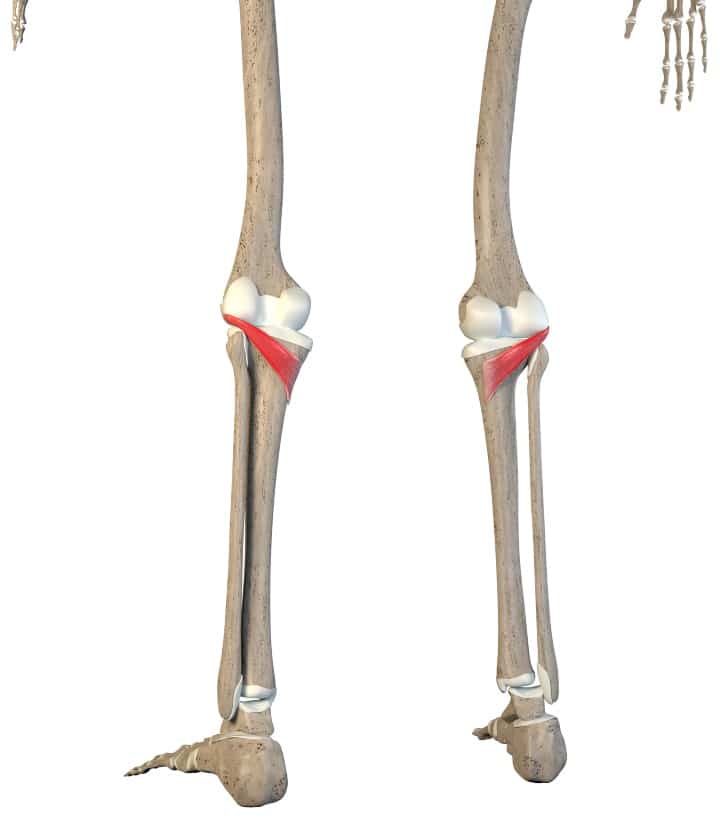
D. Popliteus
Popliteus is located in the back of the knee. It connects from the lateral femoral condyle and lateral meniscus to the back of the proximal tibia.
This muscle initiates flexion or bending the knee from a locked position.
E. Gracilis
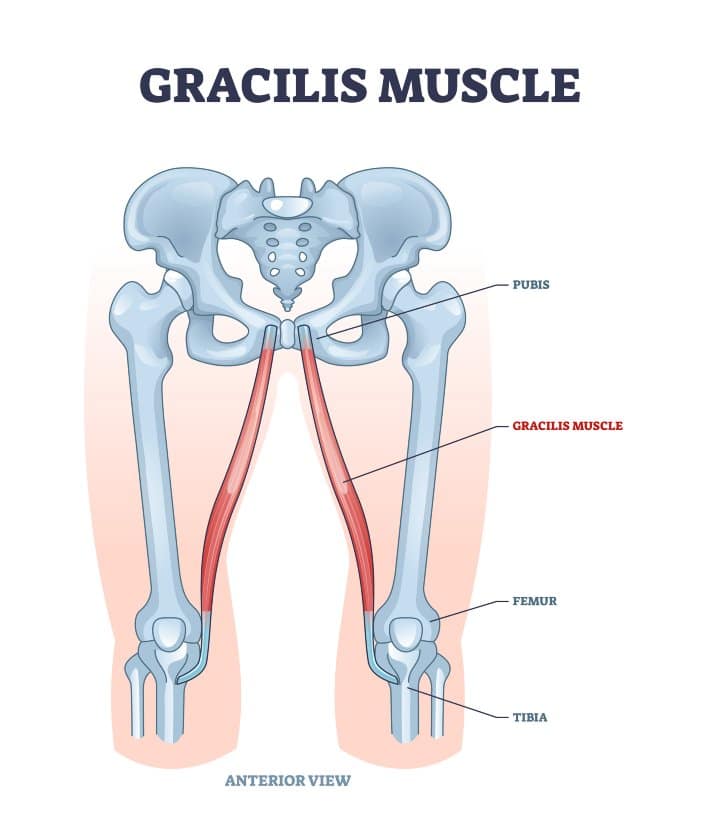
While the gracilis is primarily known for its role as a hip adductor, its crossing at the knee in the region of the pes anserine on the medial proximal tibia is worth mentioning.
When the knee is partially bent, gracilis helps with bending and internal rotation at the knee joint.
F. Sartorius
Sartorius is another thigh muscle that also crosses at the knee and attaches at the pes anserine.
Similar to gracilis, sartorius also helps with knee bending and internal rotation.
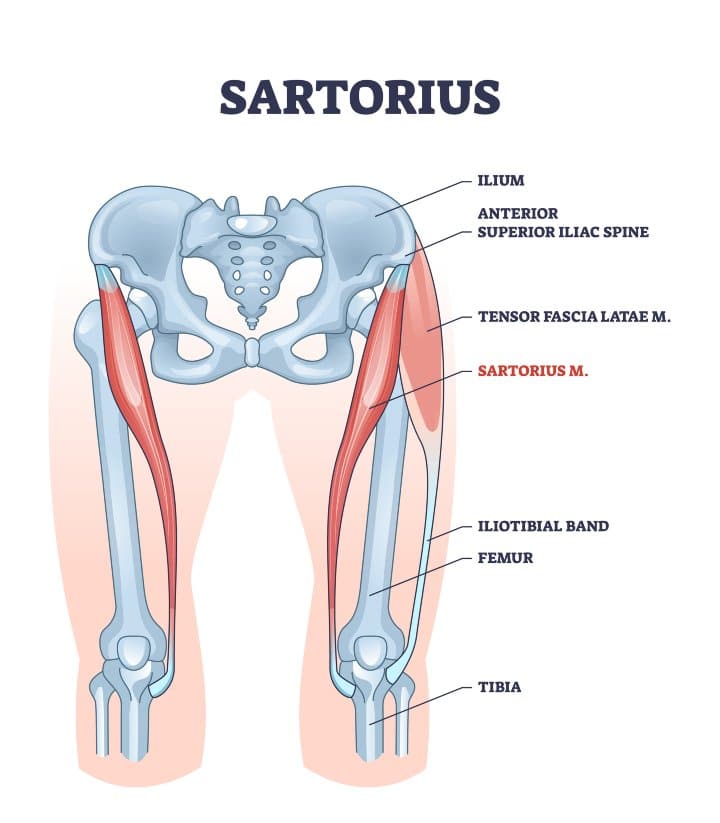
G. Tensor Fascia Latae
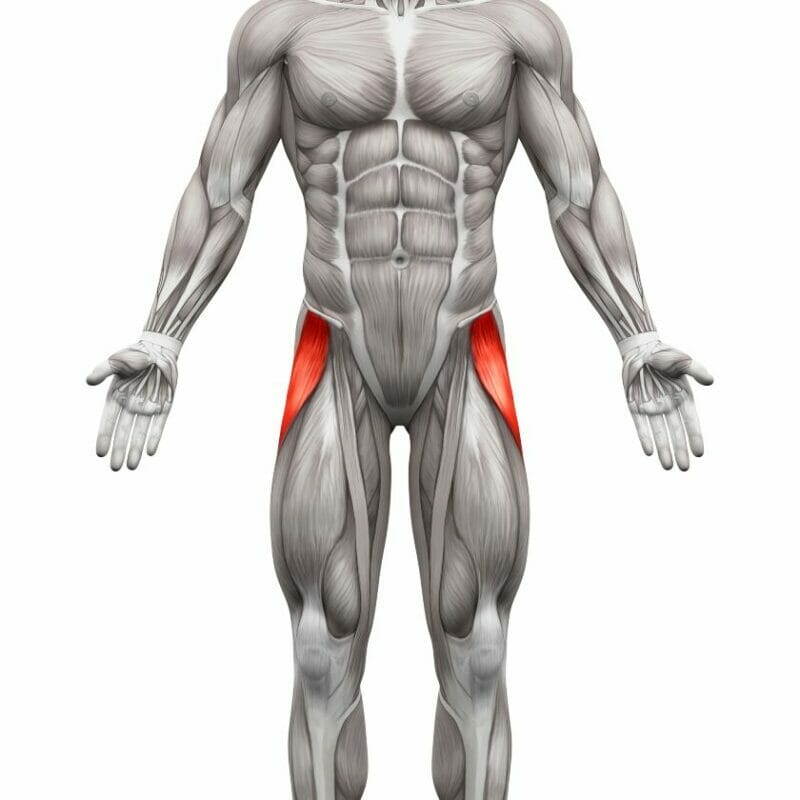
While the tensor fascia latae (TFL) is also a thigh muscle with a connection to the knee, it’s a lateral or outside thigh muscle. The previously mentioned gracilis and sartorius muscles were medial or inner thigh muscles.
The TFL connects to the lateral tibial condyle. It plays a role in lateral rotation and extension at the knee.
H. Patellar Tendon
The patellar tendon can be a little confusion because you may also hear it called the patellar ligament.
This soft tissue connects the top of the patella to the tibial tuberosity, a bone-to-bone connection which is exactly what a ligament does. This ligament though helps to improve the forces behind a quadriceps muscle contraction, which is why some will also refer to it as a tendon.
Conclusion
As you can see, there’s a lot of knee anatomy to know!
As previously mentioned, understanding the basics of knee anatomy can be very useful. Not only will it help you to know what structures support the knee, but you can use this information to help shape your workouts.
If you do happen to injure the knee or develop knee pain, knowing the knee anatomy will also help you to have a better idea of what might be happening when you seek a consult from a healthcare professional. Even better, this information can help you to prevent an injure from happening in the first place!