Free download: Top 10 Natural & Easy Remedies for Joint Pain from Home. Learn these helpful remedies.
Estimated Reading Time: 11 minutes read
Headache disorders can be incredibly frustrating to deal with. The pain can be functionally debilitating and significantly interfere with your day-to-day life.
Headache is a general term used to describe head pain, but there are actually many different types of headache categories.
Some of the most common will include migraine headaches, tension headaches, and cervicogenic headaches.
Today, we’ll be taking a closer look at cervicogenic headaches and the best ways to get rid of them.
Table of Contents
What is a Cervicogenic Headache?

A cervicogenic headache is caused by referred pain arising from the neck. This means that the true source of the pain is not actually in the head but has been radiated to the head by something going on in the neck itself.
Cervicogenic headaches are considered a secondary headache as they are caused by referred pain in the neck.
Primary headache syndromes are cases where there is no referred pain and the headache itself is the problem and source of pain.
Some of the most common causes of a cervicogenic headache will include the following issues in the cervical structures:
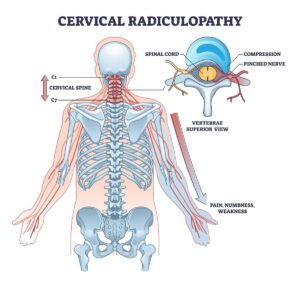
- Pinched nerves in the cervical nerve roots or another area along the cervical spinal nerves
- Whiplash injury or other neck trauma
- Rheumatoid arthritis
- Cervical disc pathology
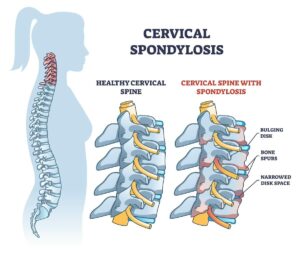
- Arthritis in the cervical vertebrae
While many headache syndromes will involve neck pain, cervicogenic headaches are specifically caused from referred pain in the neck.
Symptoms of a Cervicogenic Headache
Cervicogenic headaches tend to have distinct symptoms that help to differentiate them from other types of headaches.
Unilateral Pain:
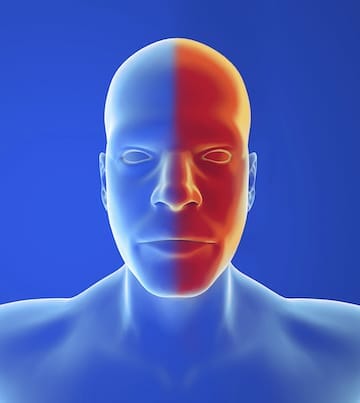
A cervicogenic headache typically will have unilateral pain, which means the pain tends to remain on one side of the head.
You may even notice this pain radiating from the base of the skull further up into the head itself.
Decreased Neck Range of Motion

It’s common to notice a stiff neck with cervicogenic headaches. You may find that specific neck movements are more challenging to move in than others.
This limited motion can be exacerbated by increased neck tension and muscle guarding due to the pain.
Unfortunately, with recurrent headaches, it’s easy to get into a nasty pain cycle. The pain you keep experiencing will naturally cause you to guard and tense.
This will further limit your range of motion and keep you from moving normally. Without normal movement, this encourages greater tension and a greater pain sensation, as well as more consistent activity from pain signals when you do then attempt to move the head and neck.
That’s why breaking the pain producing loop is so important when treating cervicogenic headaches.
Trigger Points
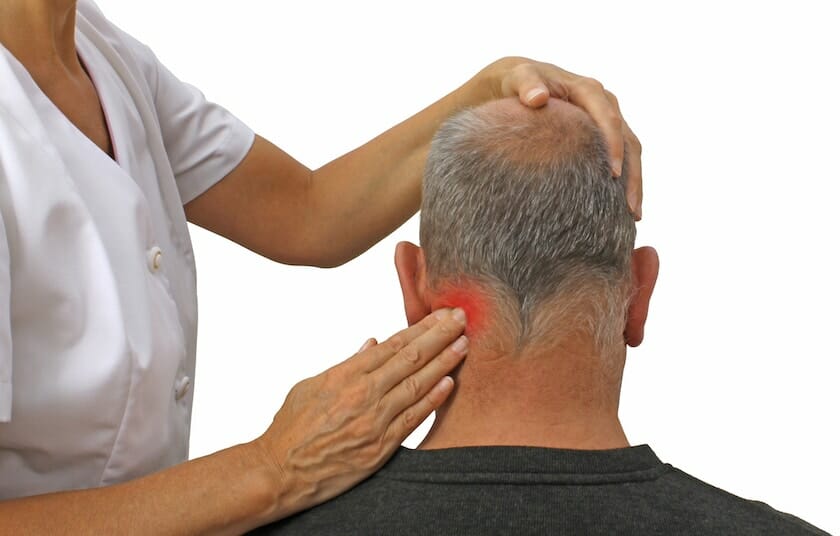
You may notice that when you press on certain spots along the neck muscles, this can re-create your cervicogenic headache.
Trigger points are focal, hypersensitive nodules that sit on a taut band of muscle. They can be active or latent. Trigger points will tend to cause radiating pain when activated.
Active trigger points are constantly triggered, with or without pressure directly on them. Latent trigger points are typically only triggered with specific pressure over them.
Red Flags: When to See a Doctor?

It’s important to note that certain signs and symptoms associated with a headache, cervicogenic or not, are considered red flags and you must seek medical attention immediately. They include the following:
- Sudden onset of severe pain
- Changes in vision, such as blurred vision, double vision or a drooping eyelid
- Dizziness
- Slurred speech
- Numbness and/or weakness on one side of the body
A cervicogenic headache must be differential diagnosed from a more severe, emergency circumstance.
It’s important to ensure that there is no evidence or occurrence of a medical emergency such as a stroke, spinal cord impingement or occlusion of important blood vessels.
If you are noticing any of the above symptoms, contact 911 immediately.
How to Help Cervicogenic Headaches
After having a formal evaluation performed by your medical doctor and a diagnosis of a cervicogenic headache is given, your doctor may suggest various treatment options.
a. Nerve Blocks
If the pain is severe enough, a nerve block may be warranted. Nerve blocks will help not only in treating pain, but also in confirming a diagnosis of a cervicogenic headache if the block is successful.
You may need this type of pain management in order to get your pain levels under control and to tolerate other recommended treatment options.
b. Physical Therapy
Your doctor will likely refer you to a physical therapist to evaluate and treat your symptoms from the cervicogenic headache.
During the evaluation, the physical therapist will be able to identify any musculoskeletal impairments contributing to your pain.
This may include as assessment of your posture, range of motion in the neck and surrounding areas, cervical and upper body strength, and any regions with tenderness when pressure is applied.
Once the evaluation is completed, the physical therapist will be able to provide a therapeutic exercise regimen for you to begin helping your cervicogenic headache and neck pain at home.
c. Posture


Poor posture can lead to muscle imbalances, causing certain muscles to become too tight and others too weak.
The most common posture to fall into is that of a forward head, rounded shoulders posture.
With regards to the neck specifically, the muscles around the cervical spine, which also attach to the base of the head, will tend to become short and tight.
This abnormal tension can lead to a tension headache or a cervicogenic headache.
Correcting the posture as a whole is important to help relieve pain from a cervicogenic headache. Otherwise, the pain cycle will continue no matter what other pain-relieving measures you try.
In relation to posture, your therapist may also ask about your workstation, especially if you’re on a computer most of the day. A poor ergonomic setup at work can contribute to poor posture, and again to your cervicogenic headache.
d. Manual Therapy
If your physical therapist notes excessive muscle tension or limited joint mobility around the cervical spine or surrounding areas, they will likely incorporate hands-on, manual therapy if you are an appropriate candidate.
Manual therapy may include massage, trigger point release, myofascial release, manual stretches, or joint mobilizations.
The goal of the manual therapy is to help reduce tension, improve soft tissue and joint mobility, and restore normal motion while providing pain relief.
e. Pillow and Mattress Support
Another factor to consider that could be contributing to your cervicogenic headache is the type of pillow and mattress you’re using.
While everyone is different, generally, you want to make sure these items are not too soft or too firm. While sleeping, you should feel that the head, neck and entire spine is supported and aligned neutrally.
Stretches and Exercises for Cervicogenic Headaches
1. Neck Stretches
If you demonstrate tight neck muscles and limited neck range of motion, you will be given a variety of home stretches to practice.
While there are many stretches to choose from, take a look at the following 2 cervical stretches directly intended to target the muscles that connect to both the neck and base of the head.
These muscles can commonly be involved in referred pain patterns and neck pain.
a. Upper Trapezius Stretch


- Starting position: This stretch can be performed seated or standing. Begin by positioning yourself in a tall, upright posture. Avoid slouching.
- If your goal is to stretch the left side of the neck, take your right hand and grab on to the top of the head.
- Gently begin pulling the head towards the right shoulder. Don’t force this motion.
- Once you’ve pulled the head as far as you can tolerate, attempt to hold for up to 30 seconds, then slowly return to your starting position. Repeat a second time.
- Repeat the entire stretching sequence on the other side.
b. Levator scapulae stretch


- Starting position: This stretch can also be performed seated or standing. Begin by positioning yourself in a tall, upright posture. Avoid slouching.
- If your goal is to stretch the left side of the neck, take your right hand and grab on to the top of the head.
- Gently begin pulling the head towards the right shoulder, similar to the upper trapezius stretch; however, this time you’ll turn the head to the right and look down towards the floor as you continue pulling. Don’t force this motion.
- Once you’ve pulled the head as far as you can tolerate, attempt to hold for up to 30 seconds, then slowly return to your starting position. Repeat a second time.
- Repeat the entire stretching sequence on the other side.
2. Neck and postural exercises
In addition to stretches to treat your cervicogenic headache, physical therapy may also require you to practice strengthening exercises.
While some of these may target the neck muscles specifically, it’s important to remember that many muscles in the neck travel and connect to areas in the shoulders and upper/mid back.
As a result, strengthening exercises may also target these areas in order to most effectively treat your cervicogenic symptoms.
Let’s take a look at 2 prime examples of exercises you may encounter while in physical therapy.
a. Chin tuck


- Starting position: You can be positioned in sitting or standing. Place yourself in a tall, upright posture with your shoulders pulled down and back.
- Gently pull the chin back as if you were trying to make a double chin. Be sure to avoid nodding the head, as if you were trying to say “yes.” Only pull the chin back as far is you can tolerate, without making the pain in the neck worse.
- Hold this position for 3-5 seconds, then slow return to your starting position.
- Repeat 10-15 repetitions for 2-3 sets.
b. Bow and Arrow


- Starting position: You can be positioned in sitting or standing. Hold the ends of a resistance band (light or medium resistance) in both hands with your arms stretched forward at shoulder height. Palms face each other.
- Picture you’re pulling back an archery bow and arrow, and that will be the motion you perform.
- One elbow, let’s say the right, will bend and begin to pull back, such as with a row.
- While this is happening, the left arm stays in its same starting position.
- As the right arm pulls back, rotate the head and upper body towards the right. Hold 2 seconds.
- Return to your starting position. Repeat on the other side.
- Alternate back and forth between sides for 10 repetitions, 2-3 sets.
Summary of Management Techniques for Cervicogenic Headaches
We’ve talked about quite a bit here!
Let’s summarize the key points for properly managing a cervicogenic headache:
- Consult with your medical doctor for an official diagnosis
- If pain is severe enough, you may require a nerve block
- Physical therapy for a full musculoskeletal evaluation and treatment plan. This will include a postural assessment, ergonomic assessment, provision of exercises, and manual therapy.
- Pillow and mattress support at home
If you’re experiencing recurrent and/or severe headaches and believe you may have a cervicogenic headache, reach out to your doctor right away.
Remember, if you notice any red flag symptoms that were listed above, contact 911 immediately.
Help is available to get your pain under control!
FAQ:
Is heat or ice better to use for my headache?
If pain is not related to a trauma or injury, you could technically use ice or heat (whichever you feel is most effective); however, if your headache is a cervicogenic headache and is related to abnormal muscle tension, you may find heat to be more effective. Heat promotes circulation and relaxation of the muscles.
What is the best pillow for the neck while sleeping?
You may have to trial different pillows before finding the right one. Make sure it’s not too soft or too hard. It should keep your head and neck in a neutral position. If you find the right one, it should help reduce morning stiffness and neck pain.
Which of my doctors should I see about my headaches?
If you are already established with a primary care physician, you may want to go ahead and schedule an office visit with them. They may choose to refer you to a neurologist for a more in-depth assessment.
If your pain is severe enough, your primary care physician and/or neurologist may also refer you to a pain management specialist.